The Role of the Nurse with the Obese Population
Obesity is considered a chronic disease in many community health texts. Community health nursing expanded dramatically during the later part of the 20th century, due in large part to a growing population of chronically ill persons (who were now surviving illnesses that were previously less treatable). This situation with the chronically ill continues to expand, shifting more and more responsibility for health management to the individual (Lundy & Janes, 2001). The role of the nurse when working with obese clients is therefore largely centered on transferring to members of this population the knowledge and skills they need to take care of themselves. To this end, nurses often take the roles of educators, counselors, advocates, researchers, and role models with obese clients.
Betty Bullock, BSN, MSN currently coordinates and instructs the diabetes education classes at the University of South Alabama Medical Center. Referring to the individuals who attend the classes, she says, "the majority of our clients are overweight, and many are obese. . . .
They generally have multiple health problems besides being diabetic, with the majority having hypertension and hyperlipidemia as well. Many of our patients have Metabolic Syndrome. This is a collection of health risks that increase a person’s chance of developing diabetes, heart disease and stroke. Since physical inactivity and excess weight are the main underlying contributors to the development of Metabolic Syndrome, becoming more physically active and losing weight can help one prevent or decrease chances of complications from this disease. Most of their health problems, if not all, could be greatly improved or maybe even cured if these patients could lose weight.
When asked about the role of "educator", Mrs. Bullock refers to interventions involving education about: the role of exercise in health maintenance, medication management and administration, nutrition and diet planning, pathogenesis of and complications from disease processes, and symptom recognition and management.
Nutrition instruction is extremely important because many of our patients believe that they can eat just about anything, and as much as they desire, as long as they stay away from concentrated sweets. Many are very surprised to learn that other foods break down into sugars, too. Teaching about portion control is another very important part of the education process. The role of exercise in helping to control blood glucose, blood pressure, and lipid levels is also emphasized.
Nursing care within the obese population also calls for the role of "counselor" in that one often implements interventions that encourage family involvement and promote self-esteem. When teaching classes such as the one Mrs. Bullock does, interventions involving the socialization of clients within support-group type environments is also very common.
The role of the educator has changed tremendously over the years . . . we are no longer just “experts” who give out information. The role has evolved into that of a facilitator who not only helps the patient to learn, but also supports them through the changes needed to best manage their disease(s). We always advise our patients to bring one other person with them to class and the rest of the participants in the class act as a support group for each other .
When working with any chronically ill population, including obese clients, nurses often find themselves playing the role of the "advocate" with many interventions involving referral to other specialists (such as dieticians, social workers, and counselors). Advocacy plays a major role due to the financial constraints that many clients face. Mrs. Bullock makes an example of the diabetes class:
The majority of our patients have no medical insurance, and little, if any, funds for medical care. They are often too old for Medicaid and too young for Medicare. We as a department and as a hospital have worked very hard to present a diabetes education class at no cost to the patient. The class is taught by: registered nurses, registered dieticians, and an exercise physiologist.
Nurses who work with the obese population often express the role of "role model"; this can be a very important role to portray with any population who depends heavily upon self-intervention to improve their health status. The nurse who presents an attitude and a set of behaviors to be emulated will be a superior caregiver within this population. Finally, the role of "researcher" is very important in order to educate the population correctly, which requires up-to-date information and evidence-based practice guidelines. In order to educate a novice on some topic, one must have accomplished a considerable level of understanding about the topic.
Primary, Secondary, and Tertiary Prevention
Primary prevention refers to the measures necessary to prevent health problems before they occur, and it involves health promotion. The purpose of primary prevention is to reduce an individual’s susceptibility to an illness by strengthening the individual’s capacity to withstand physical, emotional, and environmental stressors. Examples of primary prevention for obesity include education about proper diet and exercise before someone becomes obese. Another example is to educate people about the potential health risks of obesity (Lundy & Janes, 2001).
Secondary prevention addresses pathology, and is aimed at early detection through diagnosis. This level of prevention focuses on identifying groups of individuals who have early symptoms of disease or condition so that they can receive prompt treatment. Examples of secondary prevention for health consequences of obesity include: blood pressure screenings and blood sugar testing (Lundy & Janes, 2001).
Tertiary prevention consists of activities designed around rehabilitation. This level of prevention has a goal to restore the individual back to his/her optimal level of functioning. Examples of tertiary prevention include: regular exercise and healthy eating patterns for individuals with obesity, hypertension and diabetes (Lundy & Janes, 2001).
Sample NANDA Diagnoses for Obesity
The following NANDA diagnoses (Ralph & Taylor, 2005) are likely applicable to any client being treated for obesity:
· Imbalanced nutrition: more than body requirements
· Risk for decreased cardiac output
· Ineffective health maintenance
· Risk for activity intolerance
· Risk for chronic low self-esteem
Goals for the Client
For the diagnosis "Imbalanced nutrition: more than body requirements related to excessive intake and to socio-cultural influences which do not effectively discourage excessive intake" the following goals can be used in a plan of care:
· Client will state need to lose weight.
· Client will assist registered dietician with planning appropriate menus.
· Client will list three interventions to combat temptation and discouragement.
The individual must accept the fact that they need intervention before they can seek it. Registered dieticians will evaluate clients' eating habits, and will provide education about nutrients and foods; they will help plan individualized diets with client input. Clients will also need a plan in order to comply with their diets.
For the diagnosis "Risk for decreased cardiac output related to obesity and lack of exercise" the following goals can be used in a plan of care:
· Client will be screened for hypertension.
· Client will be screened for dyslipidemia.
· Client will be screened for diabetes mellitus.
Being overweight or obese is associated with increased risk of morbidity from hypertension, dyslipidemia, atherosclerosis, and type 2 diabetes mellitus, all of which adversely affect blood flow and perfusion. Millions of people in the United States suffer from these conditions and do not know it, so those at risk should be tested. Also, these conditions are each risk factors associated with cerebrovascular accident and decreased cardiac output due to coronary artery disease and acute myocardial infarction. Losing weight by means of a diet and exercise program reduces the risk factors for obesity related diseases (Svendsen et al. 1993; Utter et al. 1998; cited in Dick, 2004).
For the diagnosis "Ineffective health maintenance related to histories of: lack of health seeking behaviors, and lack of knowledge about disease processes" the following goals can be used in a plan of care:
· Client will verbalize knowledge concerning causation of: hypertension, elevated blood glucose levels, and elevated blood cholesterol levels.
· Client will verbalize knowledge concerning possible adverse effects of: hypertension, elevated blood glucose levels, and elevated blood cholesterol levels.
The combination of obesity and its associated morbidities adversely affects the health of obese individuals by decreasing quality of life and shortening life expectancy (Thompson et al. 1999; cited in Dick, 2004). Many clients do not know how, or why, to implement specific dietary and exercise strategies that would lower disease risk.
For the diagnosis "Risk for activity intolerance related to sedentary lifestyle and body composition" the following goals can be used in a plan of care:
· Clients will verbalize understanding of the benefits of an exercise program.
· Clients will consult a physician to determine eligibility, then plan an exercise routine.
· Clients will list three interventions to combat laziness.
The individual must accept the fact that they need intervention before they can seek it. Physicians will evaluate clients' fitness levels, and will provide education about exercise guidelines and goals; they will help plan individualized exercise routines with client input. Clients will also need a plan in order to comply with their exercise routines.
For the diagnosis "Risk for chronic low self-esteem related to negative body image and guilt" the following goals can be used in a plan of care:
· Clients will voice feelings and concerns related to obesity and its effect on self-esteem.
· Clients will participate in planning interventions and will keep a journal of efforts.
· Clients will report an increased sense of control and positive feelings about self.
Self-exploration encourages clients to consider future changes in their lives. Client input in creating diet and exercise plans will help insure compliance and a sense of control. Keeping a journal of efforts will encourage clients to assume responsibility for their own progress and will help with positive reinforcement (Ralph & Taylor, 2005).
Evidenced Based Nursing
Modern Causes of Obesity
In 2006, Dr. Margaret B. Brown of the University of Delaware Extention conducted an extensive literature review on childhood obesity prevention funded by the United States Department of Agriculture. This literature review utilized 70 research sources and a 17-member multi-state review team. Much of the background and overview information easily applies to adults as well, including descriptions of the challenging environment Americans face while being expected to maintain a normal body weight. Some of the changing characteristics of the environment that most Westerners live in today, as compared with 30-50 or more years ago:
-There is a much wider availability of inexpensive, high-calorie foods.
-There are more and more opportunities to consume food throughout the day.
-Daily activities require less energy due to automobiles, elevators and escalators, etc.
-Leisure time is more sedentary and centered around indoor activities and electronics.
-There are increasingly limited opportunities for recreational physical activity due such factors as lack of safe and open spaces, and increasing work-related time demands (Caballero, 2004; cited in Brown & Nelson, 2006).
One might add that economic forces have increased out-of-home work time for all adult family members (which results in fewer meals cooked at home); the corn and sugar industries are subsidized to the point of adding their products to just about every type of food; and advertising budgets are much larger for commercial conglomerates who produce many different types of processed convenience foods (and who generally own all levels of production), as compared with governmental agencies or smaller private agricultural groups represented by such entities as "the orange growers of the Southeast". In general, whole foods require not only preparation but refrigeration, and busy schedules away from home discourage both of these elements of healthy eating. The convenience foods that are readily available are generally much higher in added fats, sugars, sodium, and potentially carcinogenic preservatives. According to sources cited in Brown & Nelson (2006), trends in availability of food and convenience over the last 25-30 years include: increased proportion of food dollars spent away from home (Kant & Graubard, 2004); increased number of locations where ready-to-eat foods are available; preference for restaurants with limited menus, quick service, and the option for take-out; increased distribution of food through vending machines; and increased proportion of traditional offerings becoming processed (Jeffery & Utter, 2003). Furthermore, there has been a dramatic increase portion and packaging size, which began in the 1970s, rose sharply in the 1980s, and continued to increase as body weights have risen (Young & Nestle, 2002). All of these factors together have made it harder and harder to maintain a normal weight, contributing to the growing percentages of the American population who are overweight and obese over the years.
The working class are at higher risk. Although it is generally thought that the highest rates of obesity occur among population groups with the highest poverty rates and the least education, more recent research has shown that children in poor and high-income families are less likely to be overweight than children in near-poor and working class families (Hofferth & Curtin, 2005; cited in Brown & Nelson, 2006). One explanation is that, while poor families have a lower quantity of food, and high-income families have better quality food, near-poor and working-class families may have greater quantities of lower quality foods. These low cost, energy-dense/nutrition-sparse foods tend to be high in "palatable" sugars and fats and low in needed nutrition (Drewnowski & Specter, 2004; cited in Brown & Nelson, 2006). This information is easily extrapolated to adults, and it helps to explain the situation with many of the clients that community health nurses will try to help.
Evidence for Diet and Exercise as Interventions
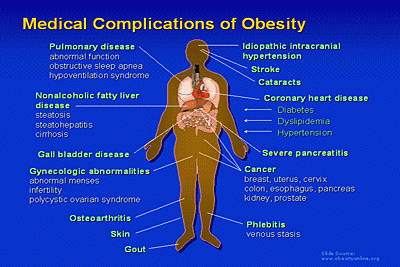
A common tool used to determine overweight or obese status is a measure of weight to height relationship known as the body mass index (BMI), which defines individuals as "overweight" who have a BMI of 25 to 29.9 kg/m2, and as "obese" who have a BMI of 30 kg/m2 or greater. In America, approximately two out of three adults is overweight, with half of these people (one out of three adults) being obese. The growing trend of overweight and obesity is considered a health condition, and it is associated with an increased risk of morbidity from: hypertension, type 2 diabetes mellitus, dyslipidemia, coronary heart disease, gallbladder disease, cerebrovascular accident, osteoarthritis, sleep apnea and other respiratory conditions, and different forms of cancer such as endometrial, breast, colon, and prostate (Rippe et al., 1998, as cited in Dick, 2004). Obesity is now the most common presenting chronic medical condition in the primary care setting (Dick, 2004).
In 2004, Jennifer J. Dick conducted a literature search to compare relative outcomes of various weight loss studies. The search resulted in identifying five clinical trials and one meta-analysis that included 493 randomized clinical trials; these trials each utilized either diet, or exercise, or diet plus exercise as interventions for weight loss in overweight and obese adult men and women. The author then critiqued and synthesized this established body of research evidence for weight loss interventions in order to bring its implications to light for use in the practice of weight-loss counseling to overweight and obese patients. The resulting implications for practice and research stem from evidence suggesting that there are various significant benefits from weight loss programs combining an energy-reducing diet together with regular exercise (despite the type of exercise). These benefits include: enhanced psychological mood (Geliebter et al. 1997; Utter et al. 1998), improved blood lipid profile (Utter et al. 1998), increased cardiopulmonary capacity (Svendsen et al. 1993; Geliebter et al. 1997; Kraemer et al. 1999), increased physical fitness and lean tissue mass (Svendsen et al. 1993; Geliebter et al. 1997), reduced risk factors for obesity related diseases (Svendsen et al. 1993, Utter et al. 1998), and maintaing a greater amount of initial weight loss at a 1-year follow-up (Miller et al. 1997) (all cited in Dick, 2004). Therefore, one implication for practice would be that health advice to obese or overweight patients should include weight loss planning that implements calorie reduction together with an exercise program.
References
Brown, M. & Nelson, P. T. (2006). What can we learn from the research literature about childhood obesity prevention?: highlights from the 2006 literature review. Retrieved November 16, 2006, from University of Delaware, College of Agriculture and Natural Resources Web site: http://ag.udel.edu/extension/fam/obesity/HiS.pdf
Dick, J. J. (2004). Weight loss interventions for adult obesity: evidence for practice. Worldviews on Evidence-Based Nursing, 1, 209-214.
Lundy, K. S. & Janes, S. (2001). Community health nursing: caring for the public's health. Sudbury: Jones and Bartlett. (532-538)
Ralph, S. S. & Taylor, C. M. (2005). Sparks and Taylor's nursing diagnosis reference manual (6th ed.). Philadelphia: Lippincott Williams & Wilkins.